What Does Herpes Look Like – Visual Guide to Stages and Symptoms
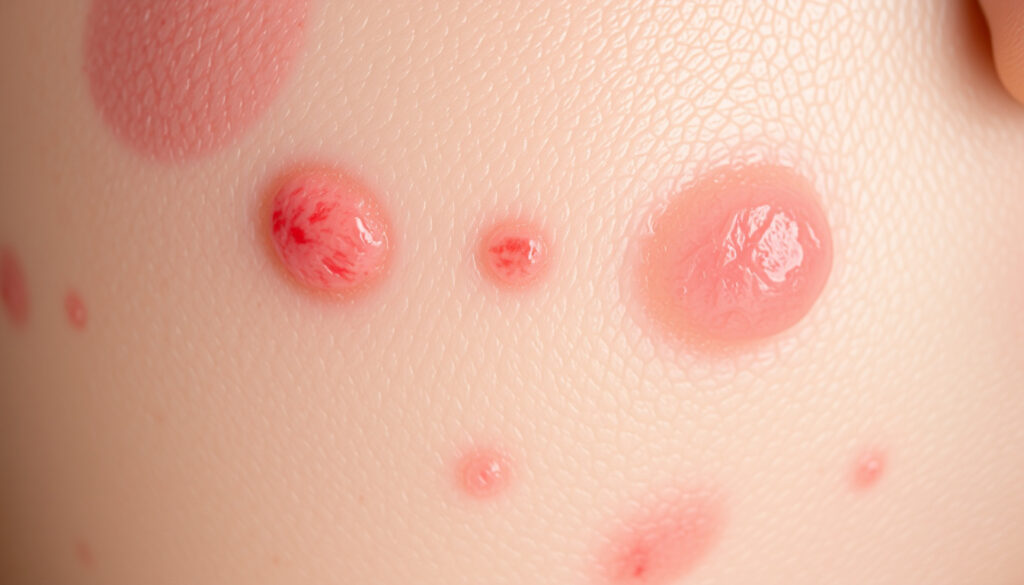
Herpes simplex virus infections present distinct visual characteristics that evolve across predictable stages. Understanding what herpes looks like can help individuals recognize symptoms, seek appropriate medical care, and distinguish the condition from similar skin issues. Both oral herpes (typically caused by HSV-1) and genital herpes (usually caused by HSV-2) follow recognizable progression patterns, though their appearance can vary based on location, skin tone, and whether it is a first or recurrent outbreak.
The Centers for Disease Control and Prevention estimates that approximately 1 in 6 adults aged 14 to 49 years have genital herpes, though many infected individuals experience mild symptoms or none at all. This high prevalence makes awareness of herpes appearance particularly relevant for sexual health. Medical professionals emphasize that visual identification alone cannot confirm herpes, as symptoms often resemble other skin conditions, making laboratory testing essential for accurate diagnosis.
This guide examines the visual characteristics of herpes infections at various stages, differences between oral and genital presentations, and how herpes compares to other common skin conditions. All information reflects established medical sources and clinical observations documented by health organizations.
What Does Herpes Look Like in the Early Stages?
Early-stage herpes often develops subtle warning signs that many people initially overlook. The prodromal phase typically begins with localized sensations before any visible changes appear on the skin.
The earliest signs of herpes include tingling, itching, or burning sensations in the affected area. These feelings typically precede visible symptoms by several hours to a full day, making them valuable early indicators that an outbreak may be developing.
Oral herpes (cold sores)
Genital herpes (sores/blisters)
Tingling, red bumps
Fluid-filled blisters
Key Insights
- Herpes often starts with itching or tingling sensations before any visible sores appear
- Blisters typically burst open, releasing fluid, and then form ulcers before crusting over
- Many outbreaks are mild or completely asymptomatic, especially in subsequent episodes
- Visual appearance varies based on immune system response and location on the body
- First outbreaks frequently include flu-like symptoms including fever and fatigue
- Recurrent outbreaks tend to be less severe and heal more quickly
- The rash may appear red or pink on lighter skin and purple or brown on darker skin tones
Snapshot Facts
| Fact | Details |
|---|---|
| Prevalence | 1 in 6 adults aged 14-49 have genital herpes (CDC) |
| Virus Types | HSV-1 (primarily oral), HSV-2 (primarily genital) |
| Incubation Period | 2 to 12 days following exposure |
| Contagious Period | During active outbreaks and viral shedding |
What Does Genital Herpes Look Like?
Genital herpes affects both men and women, though the presentation may differ slightly between sexes. The condition causes visible sores and blisters in the genital region, including the genitals, anus, buttocks, thighs, and hips. According to the Mayo Clinic, both HSV-1 and HSV-2 can cause genital herpes through skin-to-skin contact, genital fluids, or saliva.
Presentation in Men
In men, genital herpes typically appears as sores or blisters on the penis, including the shaft and glans. Lesions may also develop on the scrotum, inner thighs, or around the anus. Men may experience painful urination when sores are present near the urethra. The blisters often form in clusters on a reddened base and progress through the characteristic stages of vesicle formation, ulceration, and crusting.
Presentation in Women
Women with genital herpes may develop sores on the vulva, vagina, or cervix. According to the American Academy of Dermatology, internal sores can cause significant discomfort during urination. Lesions may extend to the perianal area, buttocks, and thighs. Women often report more extensive initial outbreaks compared to subsequent episodes.
Visual examination alone cannot confirm a herpes diagnosis. Many conditions produce similar-appearing lesions, making laboratory testing through viral culture or PCR testing essential for accurate identification.
Symptoms Affecting Both Genders
Both men and women may experience flu-like symptoms during primary outbreaks, including fever, headache, muscle aches, and swollen lymph nodes in the groin area. Pain during urination is common when ulcers are present near the urethral opening. The intensity of pain is often rated around 7 out of 10 during the vesicular stage, particularly when blisters are touched or ruptured.
What Does Oral Herpes Look Like?
Oral herpes, commonly known as cold sores or fever blisters, primarily affects the area around the mouth. The GoodRx medical team notes that these lesions typically appear on or around the lips, though they can spread to the chin, cheeks, tongue, and roof of the mouth. Most oral herpes infections result from HSV-1, though HSV-2 can also cause oral lesions through oral-genital contact.
Typical Appearance
Oral herpes blisters typically begin as small, fluid-filled vesicles that may appear singly or in clusters. The surrounding skin usually becomes reddened and sensitive. As the blisters rupture, they form shallow, painful ulcers that eventually crust over with a yellowish scab. The entire process from initial tingling to complete healing generally spans 2 to 3 weeks for primary infections.
Recurrent Outbreaks
Subsequent outbreaks of oral herpes tend to occur in the same location and are usually less severe than the initial infection. Many individuals experience warning prodromal symptoms, including tingling or itching at the site before visible blisters develop. Triggers for recurrence may include stress, illness, sun exposure, or immune system changes.
Herpes can spread to the eyes through hand contact. The American Academy of Dermatology recommends washing hands thoroughly after touching oral herpes lesions to prevent accidental transmission to the ocular area.
What Are the Stages of a Herpes Outbreak?
Herpes infections follow a predictable progression through distinct stages. According to STD Center NY, understanding these stages can help individuals recognize symptoms and take appropriate action. Each stage presents characteristic features that distinguish herpes from other skin conditions.
Timeline of an Outbreak
- Days 1-2: Prodrome Phase — Tingling, itching, burning sensations and mild pain develop. Redness and small bumps or swelling may appear. Flu-like symptoms including fever, headache, and fatigue commonly accompany primary infections.
- Days 3-5: Blister Phase — Multiple thin-walled blisters form in clusters on a reddened base. The clear or yellowish fluid inside is minimal. Pain intensity peaks during this stage, often reaching 7 out of 10 when touched.
- Days 6-8: Ulcer Phase — Blisters rupture spontaneously or from friction, releasing fluid and forming open, painful sores. A secondary crop of blisters may develop nearby. Ulcers appear as raw, moist depressions in the skin.
- Days 9+: Crusting and Healing — Sores begin to dry out, forming yellowish or honey-colored crusts. New skin gradually forms underneath. Painful urination may persist briefly. Complete healing typically requires 2 to 6 weeks for primary outbreaks.
Recurrent outbreaks generally follow the same pattern but with shorter duration and less severe symptoms. Many individuals experience only the prodromal phase without progressing to visible blisters.
How Can You Tell Herpes from Other Rashes?
Several skin conditions can resemble herpes, making visual differentiation challenging. The Medical News Today health team emphasizes that proper diagnosis requires medical evaluation. Understanding the distinguishing features can help individuals decide when to seek professional care. Other conditions that may resemble herpes include fungal infection on skin, which can present with circular, scaly patches that may itch, while herpes lesions typically burn and follow the characteristic progression through distinct stages.
Herpes vs. Pimples or Ingrown Hairs
Unlike herpes blisters, pimples typically appear as single, pus-filled bumps centered around hair follicles. Ingrown hairs develop when shaved hair grows back into the skin, causing localized irritation. Both pimples and ingrown hairs lack the characteristic clustering of herpes blisters and the pronounced burning or tingling sensation that accompanies herpes lesions.
Herpes vs. Shingles
Shingles, caused by reactivation of the chickenpox virus, presents as a unilateral rash or band of blisters following a dermatome pattern on one side of the body. The American Sexual Health Association notes that shingles typically includes severe nerve pain (postherpetic neuralgia) that differs fundamentally from the localized burning sensation of herpes. Shingles rarely appears on the genitals or mouth in typical patterns.
Comparison of Similar Conditions
| Feature | Herpes (HSV-1/2) | Pimples/Ingrown Hair | Shingles |
|---|---|---|---|
| Appearance | Clustered blisters/sores on red base | Single, pus-filled bump; possible ingrown hair | Unilateral band of blisters/rash |
| Pain/Feel | Tingling, burning, 7/10 pain | Mild soreness | Severe nerve pain |
| Location | Mouth, genitals, anus, thighs | Follicle-based, anywhere | One body side, dermatome pattern |
| Duration/Recurrence | 2-6 weeks, recurs periodically | Days, no recurrence pattern | 2-4 weeks, usually once |
| Other Symptoms | Flu symptoms with first outbreak | No systemic signs | Fever possible |
What Is Known and Unknown About Herpes Appearance?
Medical science has established clear understanding of herpes appearance and progression, though certain aspects remain variable and less predictable.
Established Information
| Confirmed Facts |
|---|
| Herpes diagnosis requires laboratory confirmation through PCR testing, viral culture, or blood antibody tests; visuals alone cannot confirm infection |
| The characteristic progression through prodrome, vesicles, ulcers, and crusting stages is well-documented |
| Clustered blisters on a reddened base distinguish herpes from single-lesion conditions |
| Primary outbreaks typically present with more severe symptoms than recurrent episodes |
| Many individuals with herpes experience no visible symptoms or very mild symptoms |
Information That Remains Unclear
| Variable Aspects |
|---|
| Exact appearance can vary significantly between individuals based on immune response and skin type |
| Recurrence frequency and severity are difficult to predict for any individual case |
| Visual appearance in asymptomatic carriers who may still shed the virus remains difficult to characterize |
| Subtle variations in appearance between HSV-1 and HSV-2 infections are not reliably distinguishable visually |
Understanding Herpes — Background and Context
Herpes simplex viruses have affected human populations throughout recorded history. The World Health Organization reports that approximately 3.7 billion people under age 50 have HSV-1 infections globally, while approximately 491 million people aged 15-49 have HSV-2 infections. These figures underscore the widespread nature of herpes infections worldwide.
While herpes cannot be cured, antiviral medications can effectively manage symptoms and reduce transmission risk. Cleveland Clinic notes that medications such as acyclovir, valacyclovir, and famciclovir can shorten outbreak duration and decrease viral shedding. Consistent use of these medications, combined with avoiding contact during prodromal symptoms and active lesions, represents the current standard for managing herpes infections.
The social and psychological aspects of herpes deserve consideration alongside physical symptoms. Many individuals experience anxiety, shame, or distress following diagnosis. Healthcare providers increasingly emphasize that herpes is a manageable medical condition rather than a personal failing, though stigma persists in many communities.
What Experts and Health Organizations Say
“Most people with herpes have no symptoms. When symptoms do appear, they typically involve small blisters that break open and crust over,” according to the Mayo Clinic.
The Centers for Disease Control and Prevention emphasizes that herpes is most contagious during active outbreaks when visible sores are present, though transmission can also occur during asymptomatic periods of viral shedding.
According to Cleveland Clinic medical professionals, early intervention with antiviral medications produces the best outcomes, particularly when started during the prodromal phase before blisters fully develop.
Next Steps and Resources
Individuals who believe they may have herpes or who have received a diagnosis should consult a healthcare provider for appropriate testing and management options. Planned Parenthood and similar organizations offer testing services and educational resources for those seeking information about herpes and other sexually transmitted infections.
Antiviral medications remain the cornerstone of herpes management, reducing both the frequency and severity of outbreaks while decreasing transmission risk to partners. Avoiding sexual contact during prodromal symptoms and active lesions, using barrier protection consistently, and maintaining open communication with sexual partners represent important complementary strategies.
For individuals experiencing symptoms that may overlap with other conditions such as Pelvic Inflammatory Disease Symptoms, seeking comprehensive medical evaluation becomes particularly important, as some conditions require different treatment approaches.
Frequently Asked Questions
Can herpes look like pimples?
While herpes blisters and pimples may appear somewhat similar, key differences exist. Herpes typically presents as clustered blisters on a red base with burning and tingling sensations, while pimples appear as single, pus-filled bumps without the characteristic viral symptoms. Recurrence patterns also differ significantly.
What does herpes look like when it first starts?
The initial stage of herpes involves prodromal symptoms including localized tingling, itching, or burning. This may be followed by the appearance of small red bumps or swelling in the affected area. These early signs typically develop 1 to 2 days before visible blisters appear.
Is herpes always visible?
No, herpes is often asymptomatic or presents with very mild symptoms that go unnoticed. Many infected individuals never develop visible blisters or sores. Asymptomatic viral shedding can still occur, allowing transmission to others even without visible symptoms.
How long do herpes blisters last?
Individual herpes blisters typically persist for several days before rupturing. Complete healing from initial outbreak to resolved scabs generally requires 2 to 6 weeks. Recurrent outbreaks tend to heal more quickly, often within 1 to 2 weeks.
What’s the difference between oral and genital herpes?
HSV-1 primarily causes oral herpes affecting the mouth and face, while HSV-2 primarily causes genital herpes affecting the genital and anal areas. However, both virus types can infect either location through appropriate contact. The appearance and progression of blisters remain essentially identical regardless of location.
Does herpes look different on darker skin?
Research indicates that herpes lesions may appear red or pink on lighter skin tones, while appearing purple, brown, or darker than surrounding skin on individuals with darker complexions. The characteristic clustered blister pattern and progression through stages remain consistent across all skin types.
Can I self-diagnose herpes based on appearance?
Visual appearance alone cannot confirm herpes diagnosis. Many conditions produce similar-appearing lesions, including fungal infections, contact dermatitis, syphilis, and non-sexually transmitted skin conditions. Laboratory testing through PCR or viral culture is required for definitive diagnosis.